Empowering Mothers: Doulas advocate for mother-friendly birth experiences
Published 4:30 am Sunday, June 2, 2019
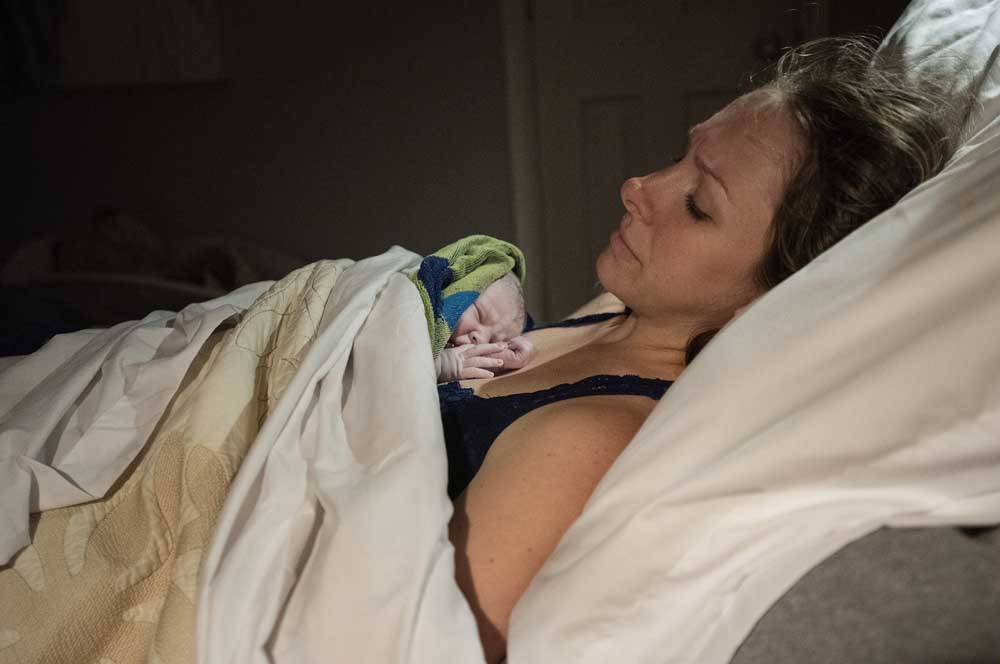
- Laura McHugh and her newborn daughter, Everly Rose, move into her bedroom minutes after birth in the living room at their house in Flint on April 2.
With supporting hands from her husband, Micah McHugh, 32, her midwife, Diane Dreier, and her doula, Gwen Spadie, Flint mother Laura McHugh, 28, gave birth to her daughter Everly Rose in the comfort of her living room. She had a birth plan, and her wishes and expectations for her birth were respected and encouraged by those in attendance at her delivery.
In the birthing pool in front of the family’s television, which was playing images of a fireplace and music from a calm, inspirational playlist, McHugh had the special experience of catching her daughter and pulling her up out of the warm water for her first breath.
“My birth was euphoric, intense, spiritual, holy and empowering,” McHugh said. “It was reassuring that birth really does go well a lot of the time, and it really can be a beautiful experience. There was something so powerful about catching my own baby that I never would have been able to experience in another setting.”
McHugh’s doula was an essential piece in her positive birth experience. She chose doula Gwen Spadie of A Sacred Nest in Tyler.
A doula is a nonmedical person who is trained to support a woman through her pregnancy. Doulas are companions who provide guidance, emotional support and comfort measures for expectant women.
Spadie applied counterpressure to McHugh’s back to help to relieve the intensity when she felt strong back labor spasms.
Spadie created the birthing space that McHugh desired. She gave supporting words reassuring McHugh that her body was working toward the birth. She helped McHugh relax and stay calm. She made sure McHugh had plenty of water to drink and fresh fruit to eat.
When the McHughs’ son Silas, 1, woke up and ran into the living room crying right as his baby sister was crowning, Spadie comforted the boy and allowed him to be a part of the birth experience.
McHugh is no stranger to the benefits of having a doula. She herself is one and the owner of Lighthouse Doula Services in Tyler.
This was McHugh’s second birth, and she chose to take the midwifery model of care instead of seeing an obstetrician and going the hospital birth route. McHugh likes the rapport that is built with having a midwife who spends the entire appointment with the mother, unlike at a doctor’s office where the patient might be seen by a nurse first and only spend a few minutes with the OB.
Midwives have training and clinical experience in childbirth. Midwives give prenatal exams and deliver the baby.
McHugh’s midwife, certified professional midwife Diane Dreier of Seeds of Grace Midwifery in Pittsburg and Longview, and the midwife’s apprentice Bri Gunter met with McHugh. The midwife did all the medical work at the birth from tracking heart tones, to taking blood pressure readings, to administering Pitocin to control bleeding after the birth, to tracking vitals for mom and baby, to delivering the placenta and checking for hemorrhage. The midwife made sure everything was medically safe for McHugh to labor at home.
McHugh’s midwife and doula were both aware of her birth plan, which included where she wanted to give birth, who would attend the birth, and what forms of intervention, if any, would be used, including pain relief. McHugh wanted to take full advantage of her home birth setting. She said having a woman’s birth team know her plan is important because sometimes when a mother is in labor, she is so absorbed in the experience that she agrees to do or not do something that was specifically in her plan. She needs the doula to keep her on track to meet her goals.
Everly Rose was born at 6:09 a.m. weighing 8 pounds, 6 ounces.
Minutes after the baby was born, the McHughs with their son, Silas, moved into the comfort of their bedroom and the bonding between baby and family instantly began.
“Our role as doulas is to be space makers,” McHugh said. “In a hospital setting the birth process can be a like a fast-moving train, but as a doula we can create space for the family. It’s such a vulnerable time in the birthing space. When you’re in labor you do what you’re told and trust who’s around you.”
The midwives and doulas stayed for several hours after the birth and met with McHugh for postpartum checkups.
Interventions
Another role of a doula is to advocate for the mother and to offer guidance when medical interventions that aren’t necessary are presented as an option.
“Typically one intervention leads to another,” McHugh said.
“When you are induced that leads to a group of interventions including constant fetal monitoring, increased intensity of contractions and it’s more likely to lead to an epidural. Once you have an epidural to block pain, you’re bedbound. You can’t move around. If you’re not up and moving you lose the natural elements of gravity and things that are shown to move birth along.”
She also warns against the artificial rupturing of the membranes to induce or accelerate labor because that puts the mother on a time frame to deliver the baby. This can lead to a failed induction that leads to cesarean section.
“C-sections have their place, they can be lifesaving, but they do have risks that can lead to death,” she said. “You have the risks that go along with surgery.”
In a situation where a doctor wants to induce, McHugh would ask the family if they would like to slow things down and have some space to talk it over.
“The doula can say, ‘Here are some questions you can ask. Is there a reason why you’re recommending that? Is it absolutely necessary? What are the risks?’” she said. “As a doula we can go over the risks and benefits and things to consider,” she said. “We are not the decision-maker, but we’re helping to create the space for the decisions to be made.”
Doulas can help a mom get out of bed and moving to help her labor continue. They can use tools such as a rebozo, a traditional Mexican garment of long, flat fabric that can be used to wrap a woman’s stomach. The rebozo can be used to help shift the baby into a better position for birth.
“We can try some essential oils; we can get you dancing,” McHugh said. “You can have your partner come and kiss you for a while to get your oxytocin flowing — there’s a lot of things we can tangibly do to help keep labor on track.”
Medical event or natural process?
The World Health Association states that since 1985, the international health care community has considered the ideal rate for cesarean sections to be between 10-15 percent. The rate of C-section delivery in the U.S. is around 30 percent.
Dr. Harsh Adhyaru, an OB-GYN physician at UT Health East Texas Physicians Jacksonville, said that the rate of C-section is high in the U.S. for multiple reasons.
“If you have a C-section once you are more likely to have all other deliveries by C-section,” he said, adding, “if you reduce primary C-sections you will reduce the overall C-section rate. If the patient has a primary vaginal delivery there’s a 95 percent chance she’ll have all other deliveries vaginally.”
Adhyaru said in the past many women were told by their OBs that their pelvis was too small to deliver a baby, but that 75 percent of those women were actually able to delivery vaginally.
Adhyaru said that with patience and giving vaginal labor a try, most women can have a natural birth.
“Everyone deserves a trial,” he said.
To decide if a C-section is medically needed there should be sufficient documentation of need due to a medical condition that might harm the mother or baby or a lack of progress in cervix dilation, Adhyaru said.
“We need good evidence of the lack of progress,” he said. “C-sections have been used quite liberally and I think they should not be.”
Even in the case of a breech baby, ultrasound guidance can turn the baby around to the optimal position with a 50 percent chance of success, he said.
The risk of having a vaginal birth after a C-section is uterine rupture, which can be lethal to mother and baby, but some hospitals are now able to offer vaginal birth after C-section (VBAC) depending on the risk factors to the patient and in-hospital staff resources.
“It’s our job to give them options,” Adhyaru said. “I list the options with her. I’ll tell her the risk of uterine rupture. I’ll tell her the risk of C-section.
“It’s the risks versus benefits options that you give the patient and they decide. It’s called informed choice in collective decision-making.”
Mother-friendly experience
Evidence suggests that the presence of a doula or nonmedical companion at birth can have a positive effect on a woman in labor, according to a 2017 committee opinion by the American College of Obstetricians & Gynecologists (ACOG), which provides guidelines for maternity care physicians.
Benefits described include shortened labor, decreased need for analgesics, fewer operative deliveries, fewer C-sections and fewer reports of dissatisfaction with the experience of labor. A woman with continuous support is also less likely to have a newborn with a low 5-minute Apgar score, which is a method of measuring the health of newborn against infant mortality.
“I don’t have to be a victim of birth,” McHugh said. “I can own and embrace and enjoy it. It’s such a powerful experience to not feel like a victim to it [pregnancy], to medicate it away or to rush it.”
McHugh loves her job as a doula. She enjoys the education side of her profession. She is trained as a doula through DONA, a nonprofit organization that provides ongoing education and professional development for doulas worldwide.
“Now I’ve seen women experience their births in unique ways,” McHugh said. “Birth matters. You can ask a woman with a 30-year-old child about the birth and she still remembers the details.”
McHugh would like to see the hospital setting become more mother-baby friendly. Some hospitals do not allow doulas to come to the delivery room, the doula can also assist the mother as she labors at home and can help her decide when it’s the right time to go.
“There’s been an emphasis on doctors knowing everything and moms are passive participants in the birth, but mom should be the most active,” she said. “A healthy baby matters, but it’s not all that matters. Women reclaiming their birthing experiences matters.”
TWITTER: @TMT_Sarah
This is Part 4 of the six-part series “Empowering Women – Improving Birth Outcomes” which focuses on personal stories of maternal health and infant mortality in East Texas as well as resources to improve maternal health and birth outcomes.
Part 1: A Tyler woman’s account of losing a child due to preeclampsia
Part 2: A Bullard couple’s account of a misdiagnosed miscarriage
Part 3: How the Glory Babies grief support group is helping parents who have lost infants or babies in utero
Part 4: How doulas are helping women be intentional about their birth experiences
Part 5: How health care providers are implementing new programs to improve maternal outcomes
Part 6: How men are learning to be more involved in parenting starting from conception
Additional articles:
- March of Dimes March for Babies raises awareness of local organizations that help expectant mothers
- Counselor addresses the grief parents face after losing a child
- Texas report shows lack of prenatal care and health insurance as barriers to healthy mothers, babies
- Christus Mother Frances Hospitals focus on maternal and infant health with expanded NICU, TexasAIM and breastfeeding policies
- Expectant Heart Pregnancy Resource Center offers free doula care to clients and also offers doula training classes
The World Health Association states that since 1985, the international health care community has considered the ideal rate for cesarean sections to be between 10-15 percent. The rate of C-section delivery in the U.S. is around 30 percent.
Studies by the World Health Association on cesarean rates conclude:
1. Cesarean sections are effective in saving maternal and infant lives, but only when they are required for medically indicated reasons.
2. At population level, cesarean section rates higher than 10% are not associated with reductions in maternal and newborn mortality rates.
3. Cesarean sections can cause significant and sometimes permanent complications, disability or death particularly in settings that lack the facilities and/or capacity to properly conduct safe surgery and treat surgical complications. Cesarean sections should ideally only be undertaken when medically necessary.
4. Every effort should be made to provide cesarean sections to women in need, rather than striving to achieve a specific rate.
5. The effects of cesarean section rates on other outcomes, such as maternal and perinatal morbidity, pediatric outcomes, and psychological or social well-being are still unclear. More research is needed to understand the health effects of cesarean section on immediate and future outcomes.






